Yes, in principle, diabetics can also get dental implants. However, successful treatment requires preparation, realistic expectations and close cooperation between the dentist and the diabetologist. From a clinical perspective, the most critical parameter is HbA1c. Well-controlled diabetes – typically reflected by an HbA1c value within the target range recommended by the patient’s physician – significantly improves healing capacity and reduces post-operative complications. We encourage patients to share recent laboratory results before implant placement, and in some cases, we liaise directly with their medical team. Timing of surgery, antibiotic coverage, minimally invasive techniques and strict follow-up protocols all play a role. When these elements are aligned, the success rates of dental implants in controlled diabetic patients approach those of non-diabetic individuals. between the dentist and the diabetologist are necessary. For the procedure to be successful and avoid complications, certain important factors must be taken into account. Careful medical history, assessment of periodontal status and radiographic evaluation of bone volume form the foundation of safe treatment planning. We never rush this phase. Good preparation often determines long-term success more than the surgery itself. More info about the
timeline of tooth implantation.
Bone grafting: necessary?
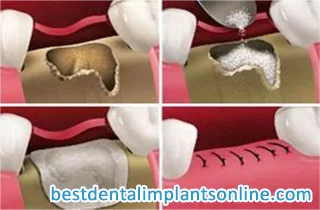
Bone grafting may also be required for this implantation procedure. The extent of the existing bone loss is important here. The surgeon decides individually whether bone reconstruction should be carried out or not.
In patients where diabetes and dental implants intersect, bone quality deserves special attention. Long-standing diabetes may subtly affect bone metabolism and turnover. If CBCT imaging reveals insufficient bone height or width, guided bone regeneration or sinus lift procedures can be performed safely, provided glycaemic control is stable. We often recommend a staged approach in more complex cases. First, eliminate active periodontal infection. Second, rebuild bone if necessary. Third, place implants under controlled conditions. This structured pathway minimises biological stress and gives tissues time to respond predictably.
Requirements for dental implants for diabetics
Good blood sugar control: Stable blood sugar control is the key to a successful implantation. Advantages: Well-controlled blood sugar supports the healing process and reduces the risk of complications. A stable blood sugar level strengthens the immune system, protects against infections and increases the chances of success and the longevity of dental implants.
Regular oral hygiene: Thorough oral hygiene is essential to minimise the risk of infection. Twice-daily brushing with a soft brush, interdental cleaning and professional hygiene visits every 3–6 months are not optional extras; they are part of the treatment. In diabetic patients especially, plaque control directly influences implant prognosis.
Smoking cessation: If the patient smokes, we strongly advise quitting before implant placement. Smoking combined with poorly controlled diabetes significantly increases implant failure risk.
Maintenance protocol: Scheduled recalls with radiographic monitoring help detect early bone changes around implants. Early intervention can prevent major complications.
Although diabetes poses a challenge to the success of dental implants, it is not an absolute obstacle. With good blood sugar control, careful oral hygiene and close cooperation between dentist and diabetologist, diabetics can also benefit from the advantages of dental implants.
Benefits of dental implants for diabetics
Improved quality of life: Stable, fixed teeth restore chewing efficiency, which is particularly important for diabetic patients who must follow a balanced diet. Being able to chew fibre-rich vegetables or protein sources properly supports metabolic control.




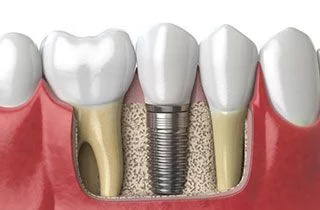 When discussing diabetes and dental implants, the distinction between controlled and uncontrolled diabetes is crucial. Uncontrolled diabetes – persistently high HbA1c, frequent hyperglycaemic episodes – represents a temporary contraindication. In such cases, we postpone surgery and refer the patient back to their physician. Implant therapy is elective. Safety comes first.
When discussing diabetes and dental implants, the distinction between controlled and uncontrolled diabetes is crucial. Uncontrolled diabetes – persistently high HbA1c, frequent hyperglycaemic episodes – represents a temporary contraindication. In such cases, we postpone surgery and refer the patient back to their physician. Implant therapy is elective. Safety comes first.